Benign prostate hypertrophy, abbreviated as “BPH,” is a common condition where the prostate grows large enough to cause troublesome urinary symptoms. Some men may find their urine stream to be weaker, notice it takes a longer time to empty their bladder, or have a feeling of incomplete bladder emptying. In very serious cases, patients may not be able to urinate at all.
There are multiple ways to alleviate your symptoms. Your provider may suggest one of the following options: Lifestyle Changes, Medications or Surgery and other procedures.
Lifestyle Changes
In certain cases when you are unable to pee, or have a lot of urine retained in your bladder after you void, you may need to make lifestyle changes. This may include learning how to catheterize yourself a few times a day to completely empty your bladder, or have an indwelling foley catheter.
Medications
There are three main categories of medications that can help with BPH: alpha blockers, 5 alpha-reductase inhibitors, and PD5-inhibitors. Alpha blockers help with the flow and stream of your urine. 5 alpha-reductase inhibitors shrink your prostate over time. PD5 inhibitors can help with both erectile dysfunction and reduce prostate inflammation to help with urinary symptoms. These medications will likely need to be taken life long.
Surgery and Other Procedures
Depending on your health history, you may be a candidate for surgery. You will need to complete additional testing prior to being considered for surgery, such as undergoing imaging of your prostate and a cystoscopy. There are different surgery options depending on your prostate size, including but not limited to: Urolift, Rezum, transurethral resection of the prostate (TURP), and holmium laser enucleation of the prostate (HoLEP). These procedures have different rates of effectiveness and side effects. If surgery is not a good option for you, you may be recommended to have a prostate artery embolization (PAE), which helps shrink the prostate over time.
Once you have discussed your concerns with your medical provider, you may be prescribed medications to treat your symptoms. Click here for the main categories of medications.
Alpha Blockers
These medications help relax the smooth muscle of your prostate, improving the channel that your urine flows through. They do not change the size of the prostate. The most common medication that is prescribed under this category is called tamsulosin. You should be able to feel the benefits right away. A common side effect is dizziness. Some patients may experience retrograde ejaculation - also known as a dry ejaculation. If these are bothersome side effects, let your provider known, there are other options to consider.
Alpha-Reductase Inhibitors
These medications help stop the enzymes that convert testosterone into the primary hormone that feeds the prostate. Over time, the prostate will shrink which will improve urinary symptoms. However, it may take 3-6 months to notice any effect. This category of medications work best for those with larger prostate. The most common medication that is prescribed under this category is called finasteride. A small number of patients may have difficulty with erections as a side effect.
PD5-Inhibitors
These medications help with both erectile dysfunction and symptoms of BPH by relaxing the smooth muscle fibers of your bladder and prostate. The most common one prescribed is called tadalafil and it is a daily pill. Side effects may include runny nose and headache.
Click here for surgical options and to learn what you can expect leading up to surgery, during your procedure, and your recovery.
HoLEP
HoLEP is a procedure that uses a laser to remove prostate tissue that is blocking urine flow, without requiring any incision. Like removing the fruit in an orange and leaving behind the peel, a laser will remove a significant porti e under general anesthesia and asleep for this entire procedure.

Preparing for Surgery
Once you have decided on surgery, you will be contacted by our surgery coordinator for scheduling. Then there will be a few things you may have to complete:
1. You may be asked to complete some blood work, if you have not done any recently
2. You will be asked to submit a urine sample, if you have not submitted one within 30 days of surgery
3. You may be asked to schedule your COVID test within four days of your surgery date
4. You will be contacted by the Prepare Clinic 1-2 days before surgery to answer any questions. If you do not receive a call, please notify the clinic for additional instructions Generally, you should not have anything solid to eat 8 hours before your surgery and can take small sips of water up to 4 hours before your surgery
5. You will be asked to arrive in the Pre-Op unit two hours before the time your surgery is scheduled to start
During the Procedure
Your surgery is expected to take a few hours. You will be completely asleep for the procedure. You will wake up with a foley catheter, which is a tube that drains your bladder. It is important for us to monitor the color of your urine after surgery. If there is not a lot of blood in your urine (hematuria), you may be able to go home the same day and return to clinic to have it removed, about 5-7 days, by your provider.
Follow-Up
If your foley catheter was removed while in the hospital, expect a telehealth follow-up in approximately 4-6 weeks to check in with your surgery team. Afterwards, expect an in-person follow up in clinic in 2-3 months for a flow rate study and bladder scan ultrasound. Be ready to urinate during this visit.
Recovering after Surgery
The recovery from HoLEP varies from individual to individual. Factors that may influence healing time include age, preexisting urinary symptoms, other health conditions and medications.
Listed are some general expectations after a HoLEP:
• Better urinary flow
• Burning sensation during urination, as urine passes through a freshly operated area, which can be managed with over-the-counter medications such as Tylenol and Pyridium
• Blood and blood clots in your urine that comes and goes for about eight weeks as the prostate heals
• Temporary urinary leakage, lasting weeks to months
• Retrograde ejaculation is expected
Diet and Activity
• No lifting anything greater than 10 pounds for 4 weeks
• Avoid any straddling activities (biking, motorcycles, horseback riding, etc.) for 4 weeks
• Keep hydrated with fluids, 2.5-3 liters to keep urine clear and to flush any blood clots
• Prevent constipation with over-the-counter stool softeners and laxatives, such as Colace or Miralax
• No hot tubs or hot baths for 4 weeks
When to Call the Clinic
• Fever, temperature greater than 101 degrees Fahrenheit
• Intolerable pain
• Not being able to urinate
• Thick blood in the urine
Rezῡm
Rezῡm is a minimal invasive treatment that uses steam to remove excess prostate tissue (less than 80 grams). As your body absorbs the treated tissue, shrinking the prostate, opening the urethra, while reducing bothersome urinary symptoms. Symptom relief is experienced as soon as two weeks with maximum occurring within three months.
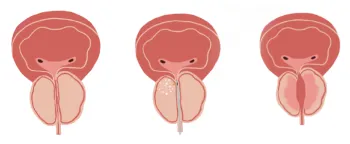
Advantages of Rezῡm
• Preserve sexual function
• Lower chances of retrograde ejaculation in comparison to other prostate procedure
• Lasting results for about five years
Preparing for Rezῡm
• Blood and urine test prior to surgery
• Stop anticoagulants or blood thinners a week before the procedure
Day of the procedure
• Rezῡm is often performed in our Outpatient Surgical Center, meaning you can go home same day
• Plan on spending approximately two hours for the entire procedure
• You will have a temporary foley catheter in place
• Since you will be under general anesthesia, plan on transportation home
Recovering after Rezῡm
• Resume your anticoagulation in two weeks or as instructed by your doctor
• Urinary symptoms get worse before they better
• Some may experience temporary painful urination, urinary frequency and urgency, blood in urine or semen, urinary retention, and pelvic pain
• Avoid activities that may irritate you
PAE
Prostate artery embolization reduces the blood supply to the prostate and shrinks the prostate gland over time. Using x-ray guidance, a small tube called a microcatheter is advanced into the prostatic arteries, where small beads are injected to block the blood flow. The procedure takes 2-3 hours, and patients go home the same day.
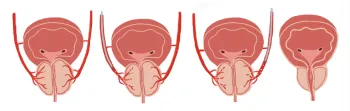
Advantages of PAE:
• Low risk of sexual dysfunction
• Option for patients who want to avoid a procedure through the urethra
• Works especially well in very large prostates (80 cubic centimeters or greater)
Disadvantages of PAE:
• May need repeat PAE or another surgical procedure at five-year mark, as prostate regrowth can occur over time
• Improvement in BPH symptoms usually not noticeable until 3-4 weeks after the procedure
Preparing for PAE
• Blood tests within 1 month of the procedure
• If applicable, your anticoagulants may be stopped several days prior to the procedure, however we may opt to continue these medicines on a case-by-case basis
• PSA lab within 3 months
Day of your procedure
• PAE is performed in Interventional Radiology at the UCSF Parnassus campus, and patients are discharged the same day
• Plan on spending approximately six hours with us on the day of the procedure, this includes: 1 hour of preparation, 2–3-hour procedure time, and 2 hours post-procedure to ensure that the vessel access site is free of significant bleeding
• A small dissolving plug will be used to close the vessel if the procedure is performed from the common femoral artery in the groin and compression band will be applied to the wrist if the procedure is performed through the radial artery in the arm
• Since you will be under sedation for the procedure, plan to arrange transportation home
Recovering after PAE
Patients may experience symptoms after PAE including:
• Burning/pain with urination for about 1-2 weeks
• Increased frequency and urgency to urinate for several days to a week
• Sudden painful contractions of the bladder, which may be relieved by a medication called oxybutynin
• Blood-tinged urine, semen, or stool for 1-2 weeks
• Bruising at the puncture site
• No sexual activity for 1 week
Medicines prescribed for recovery include:
• A course of antibiotics to prevent urinary tract infection
• Anti-inflammatory agents (ibuprofen, methylprednisolone) to reduce the irritative symptoms above
• Bladder relaxant (oxybutynin) only as needed for bladder spasms, monitor for inability to urinate
Notify us for:
• Continued bleeding or worsening bruising at the vessel access site
• Discomfort not controlled by provided medication
• Inability to urinate
• Upon completion of the procedure, you will be provided with daytime and overnight numbers to call should you have any issues!
Urolift
Urolift is a minimally invasive procedure that uses implants to permanently lift and hold the enlarged prostate tissue out of the way and increase the opening of the urethra. You may be a suitable candidate for this procedure if your prostate is between 30-80 grams and your prostate does not have a median lobe, which will be determined by your surgeon.
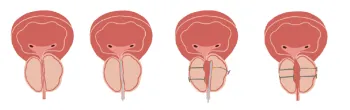
Advantages of Urolift:
• No changes to sexual dysfunction or erectile dysfunction
• Rapid improvement in lower urinary tract symptoms and quality of life
Disadvantages of Urolift:
• May need additional surgery at the five-year mark or take medications again
• May not be suitable for certain MRI tests, patients will be given an implant card
Preparing For Surgery
This procedure is often done in an outpatient setting. You will be given local anesthesia and it will take less than an hour.
Recovering After Procedure:
You may experience some burning with urination and blood in the urine after the procedure, which is normal. Most individuals can return to work in 2-3 days.
Important Contact Numbers
During Monday through Friday, 8 AM - 5 PM, questions can be directed to the following:
Parnassus Urology Clinic: 415-353-2200
Redwood Shores Urology Clinic: 415-476-7877