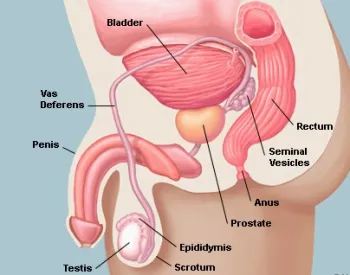
Testicles are two egg-shaped structures with a firm, slightly spongy feel located below the penis in the sac of loose skin called the scrotum. The size of the testicles should be roughly the same. Two main functions of the testicles include sperm and testosterone production. Tumors of the testicle are relatively rare malignancies, accounting for 1-2% of cancers among US men, with an incidence of approximately 5.4 out of 100,000 men per year. The incidence is highest in Caucasians and lowest in African-Americans. Risk factors for developing testicular cancer include a history of cryptorchidism (i.e. one or both testicles failed to move into the scrotum before birth), family history of testicular cancer, and a personal history of testicular cancer. Most testicular tumors are initially diagnosed due to discovery of a painless firm mass in the testis. After consultation with a physician, this may be confirmed with an ultrasound of the testicle, which is a simple non-invasive radiologic procedure. At the time of diagnosis, blood tests should be obtained to measure serum tumor markers which are essential in the diagnosis, prognosis, and monitoring of testicular cancer. The initial treatment option for testicular cancer involves surgery to remove the testicular tumor and its affected testicle, which is called a radical orchiectomy. It is performed through a small incision in the groin. This procedure is performed for definitive diagnosis and staging, but also it can also be a highly effective treatment. Further treatment, if any, will depend on the type of tumor found during orchiectomy and can include surveillance (i.e. periodic blood tests and x-ray tests), surgery, chemotherapy, or radiation therapy. The good news for testicular cancer patients is that an effective strategy employing surgery, chemotherapy, or radiation in an appropriate manner has produced cure rates between 95-99% for low stage, early disease.










