Prostate Cancer
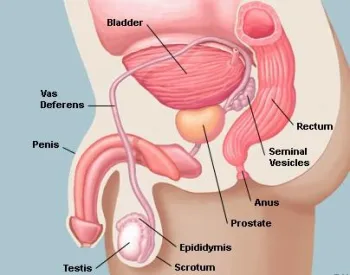
About Prostate Cancer
Prostate cancer is the second most common cancer (following skin cancer) in U.S. men and is the second leading cause of cancer death in men. One in nine men born in the U.S. today will be diagnosed with prostate cancer during his lifetime. The risk of dying from prostate cancer, however, is much lower, at one in 41. Your individual risk depends on your risk factors. Learn more at Understanding Prostate Cancer.
Each individual person's journey with prostate cancer can vary. With this in mind, the Patient Services Committee in collaboration with UCSF Physician Scientists in Urologic Oncology, Medical Oncology, and Radiation Oncology have developed prostate cancer education materials to help guide conversations for you and your physician.

UCSF Health Prostate Cancer Center
The UCSF Prostate Cancer Center offers advanced, comprehensive care for individuals diagnosed with prostate cancer and those at elevated risk for the disease. Prioritizing early screening and detection, our center provides a wide array of services, from active surveillance for low-risk cancers to innovative treatments for cancers at all stages, whether localized (restricted to the prostate) or advanced (metastasized beyond the pelvis). UCSF is a prominent research institution for late-stage prostate cancer, providing access to the most effective treatment options.
News
Related Providers
Clinician Faculty

Peter R. Carroll, MD, MPH
- Professor of Urology
- Ken and Donna Derr-Chevron Distinguished Professorship in Prostate Cancer

Meera R. Chappidi, MD, MPH
- Assistant Professor of Urology

Carissa Chu, MD
- Assistant Professor of Urology
- Stephen and Faith Brown Endowed Professorship in Urology

Matthew R. Cooperberg, MD, MPH
- Professor of Urology
- Professor of Epidemiology and Biostatistics
- Helen Diller Family Chair in Urology
- Research Council Chair
- Chief of Urology, San Francisco VAMC
- Co-Leader, Prostate Program, HDFCCC

Maxwell V. Meng, MD
- Professor of Urology
- Vice Chair of Quality and Safety

Hao G. Nguyen, MD, PhD
- Associate Professor of Urology
- Richard and Leilani Grinold Endowed Professorship in Urology

Anobel Y. Odisho, MD, MPH
- Associate Professor of Urology
- Associate Professor of Epidemiology and Biostatistics
- Director of Clinical Informatics and Digital Transformation
- Medical Director of Surgical Informatics at UCSF Health

Sima P. Porten, MD, MPH
- Associate Professor of Urology
- Chief of Urologic Oncology

Rishi R. Sekar, MD, MSc
- Assistant Professor of Urology

Katsuto Shinohara, MD
- Professor of Urology
- Helen Diller Family Chair in Clinical Urology

Samuel L. Washington III, MD, MAS
- Assistant Professor of Urology
- Goldberg-Benioff Endowed Professorship in Cancer Biology
- Associate Chair of Inclusive Excellence
Courtesy Faculty



Franklin Huang, MD, PhD
- Associate Professor of Medicine and Urology

Michael Rabow, MD, FAAHPM
- Professor of Medicine and Urology
- Helen Diller Family Chair in Palliative Care

Mack Roach III, MD
- Professor of Radiation Oncology and Urology

Eric Small, MD
- Professor of Medicine, Hematology Oncology and Urology
- Doris and Donald Fisher Distinguished Professorship in Clinical Cancer Research
- Stanford W. Ascherman and Norman R. Ascherman Endowed Chair
Researchers

June M. Chan, ScD
- Professor of Epidemiology and Biostatistics and Urology
- Steven and Christine Burd - Safeway Distinguished Professor

Nynikka Palmer, DrPH, MPH
- Assistant Professor of Medicine (Division of General Internal Medicine at SFGH), Urology and Radiation Oncology
- Helen Diller Family Chair in Community Education and Outreach for Urologic Cancer

Donna Peehl, PhD
- Professor of Radiology and Urology
Pathologists

Cornelia Ding, MD, PhD
- Assistant Professor of Pathology and Urology

Physician Assistants


Sara McRorey, PA
- Physician Assistant
Nurse Practitioners